
Malaria
Treatment and Research

Tuberculosis
The fight against tuberculosis.

HIV - AIDS
Treatment
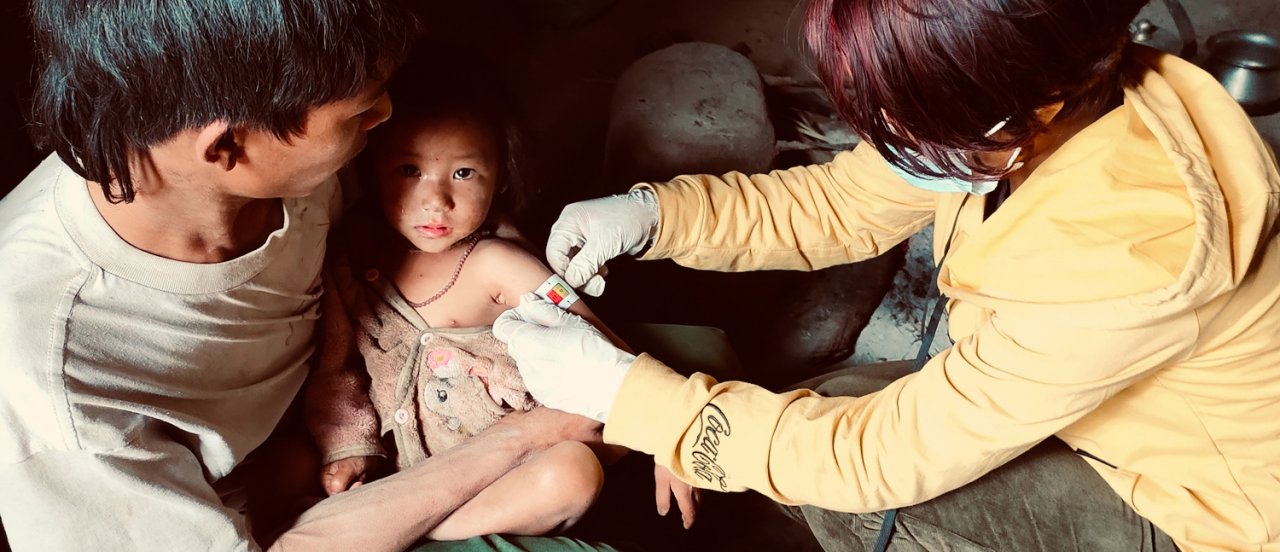
Malnutrition
Screening for malnutrition in children and pregnant women

Rickets
Bone deformity in young children

Sexually transmitted infections and Family planning
Improving health and lowering risks.

Referrals
Patients with complicated diseases are referred to other hospitals at the costs of MAM.

COVID-19
COVID-19 epidemic
